LMIC Operating Room Equipment Survey
Summary
Using our existing network of Biomedical Engineers, we surveyed 75 operating rooms across 7 LMICs. We created suitable, realistic benchmark standards that every operating room should meet to be considered safe. These standards reflect the challenges of providing healthcare in the LMIC environment.
Of the 75 operating rooms, not a single one can be considered safe, i.e. meeting all our benchmark standards across all sections.
The proportion of healthcare facilities that passed our benchmark standards for each section (in descending order) were as follows:
- Oxygen – 100% (due to Covid highlighting the need for oxygen).
- Sterilisation – 90% (due to lack of functioning autoclaves).
- Anaesthetics – 49% (mainly due to lack of soda lime replacement and poor monitoring).
- Patient Monitoring – 40% (mainly due to lack of child and neonate sized accessories).
- Operating Tables – 10% (due to a lack of necessary accessories, and electric operation).
- Suction – 4% (due to lack of battery backups).
- Lighting – 0% (due to a lack of battery backups).
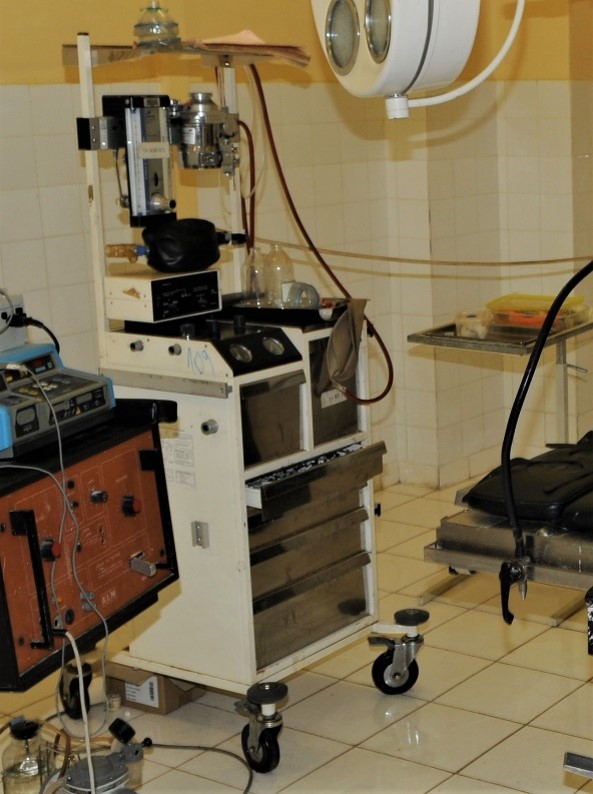
Modified, unsafe anaesthetic machine with no patient monitoring.

An open circuit anaesthetic machine designed for the LMIC environment.
Above is just one example of poor operating room conditions in LMICs that we see on a regular basis. Sadly, dangerous setups such as these cost lives. During the writing of this report, an otherwise healthy child was tragically lost during a straightforward operation due to poor operating room conditions.
This data in this report is aims to shed light on the terribly under resourced operating rooms in LMICs, as well as offering solutions about how to resolve these issues. In brief, it comes down to suppling suitable equipment that is tailored to the LMIC region, alongside biomedical engineering training to maintain the equipment in the long term.
Our comprehensive, 50+ page report discusses all key aspects of equipment in LMIC operating rooms including sterilisation practices, anaesthetics, patient monitoring, operating tables, suction, oxygen and operating lights. Below is an extract of the operating room lights section of the report. For this section, the benchmark standards considered were:
- All bulbs must be working correctly, maximum illumination is required to allow the surgeon to optimally perform their task.
- There must be no drift, this means the light will stay where it is needed – allowing the surgeon to focus on their task rather than becoming distracted with repeatedly repositioning an operating room light.
- A battery backup must be present, this is to allow surgery to continue in a power cut.
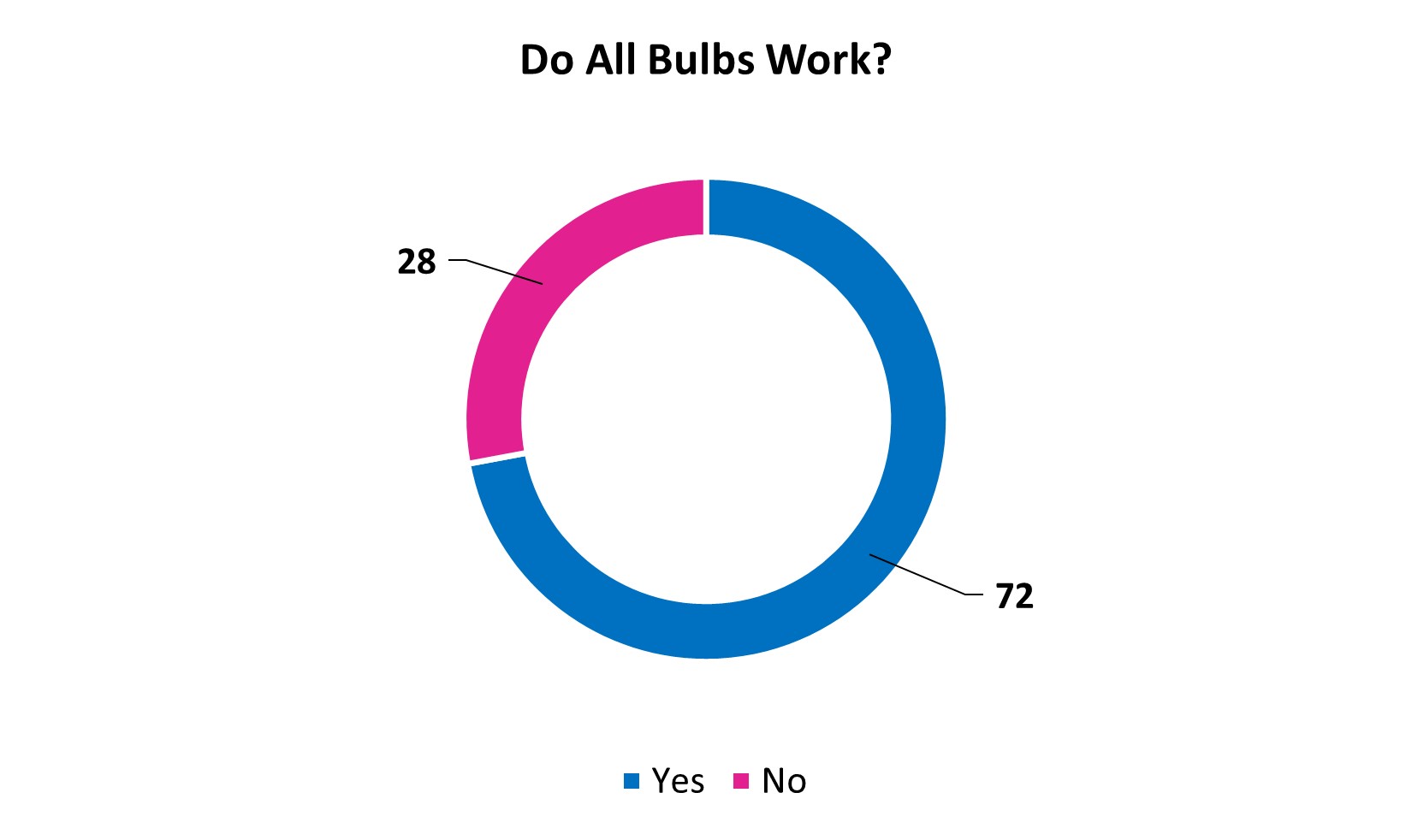
Proportion of operating room lights with all bulbs working, across operating rooms in LMICs (in %).
Only 72% of operating room lights are working correctly, i.e. with all bulbs working. This presents challenges during surgery as the surgeon will not have optimal lighting in order to perform their role to the best of their ability.
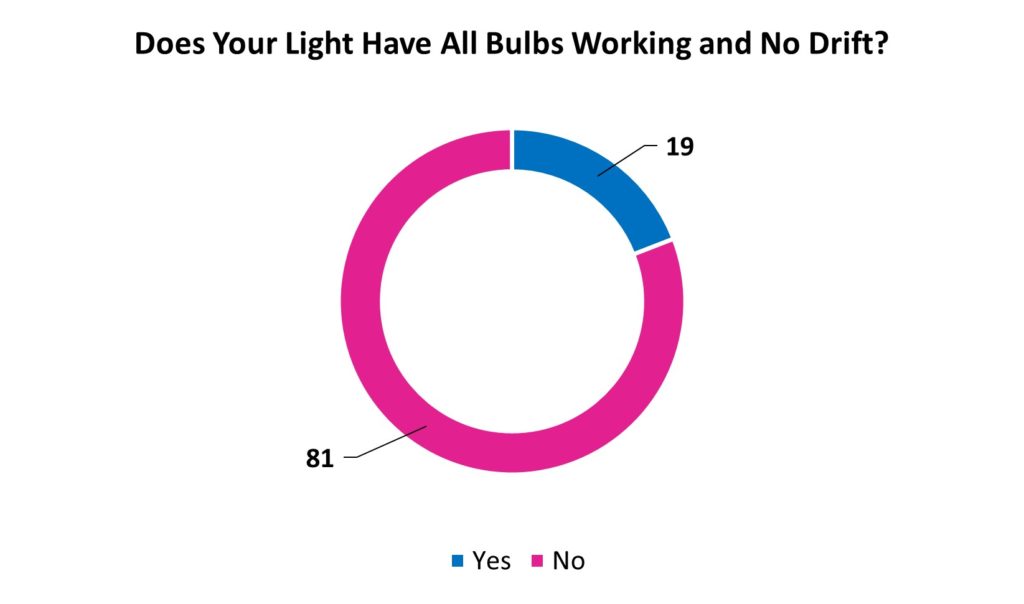
Proportion of operating room lights with all bulbs working, and that do not suffer from drift, across operating rooms in LMICs (in %).
When considering if the operating lights have all bulbs and working as well as having no drift, only 19% are suitable. The fact that many lights also drift means the surgeon will be distracted trying to manoeuvre the operating room light into the correct position. This is far from ideal for conducing safe surgery.
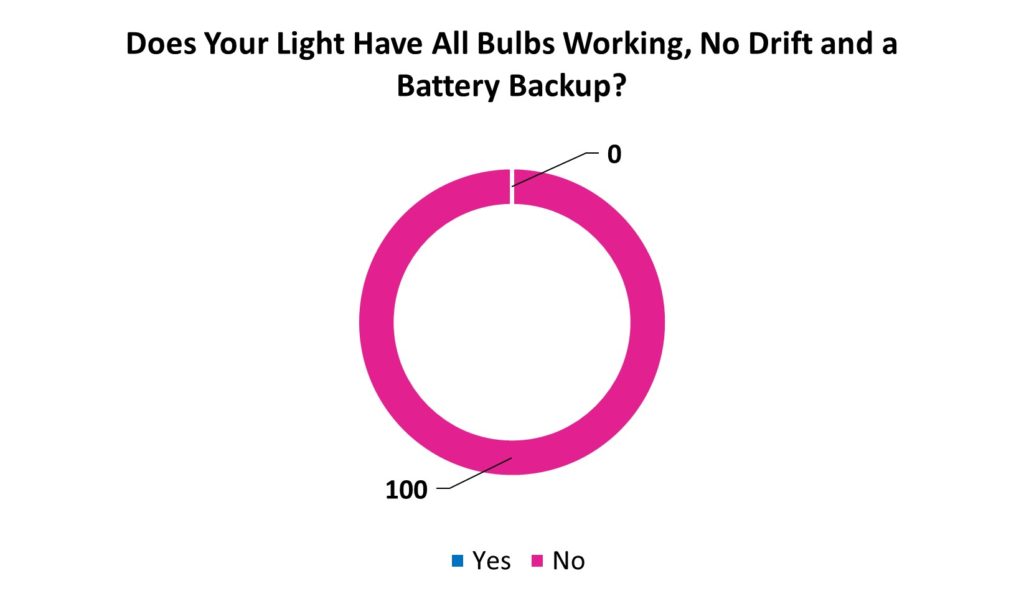
Proportion of operating room lights with all bulbs working, that do not suffer from drift, and have a battery backup, across operating rooms in LMICs (in %).
In order to protect against power outages, which are particularly common in LMICs, a battery backup is essential to ensure surgery can continue. None of the 75 operating room lights surveyed met all 3 benchmark standards: having all bulbs working, no drift, and a battery backup. This is a very concerning finding.
Please click the link below to access the full report. It discusses the many challenges faced in LMIC operating rooms, whilst offering possible solutions.

